Oral and Maxillofacial Surgery
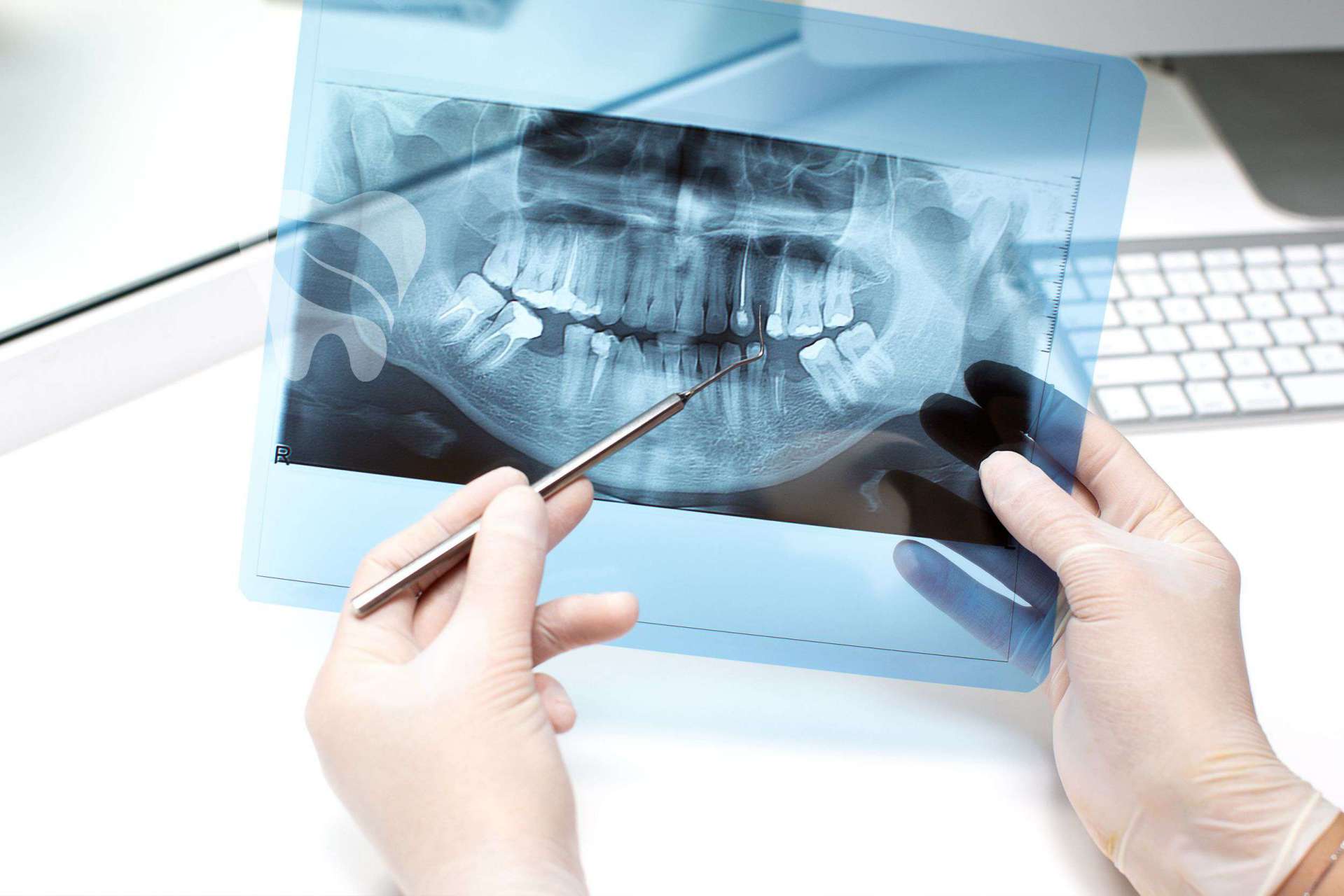
Oral and maxillofacial surgery is the specialty dedicated to diagnosing and treating conditions affecting the mouth, teeth, jawbones, temporomandibular joint, and surrounding soft tissues. At Yaprak Dent we assess every patient comprehensively and combine advanced imaging with a multidisciplinary approach to deliver individualized surgical plans. Depending on the complexity of the case, procedures are performed under local anesthesia, conscious sedation, or general anesthesia in fully sterile operating-room conditions.
Treatments We Offer
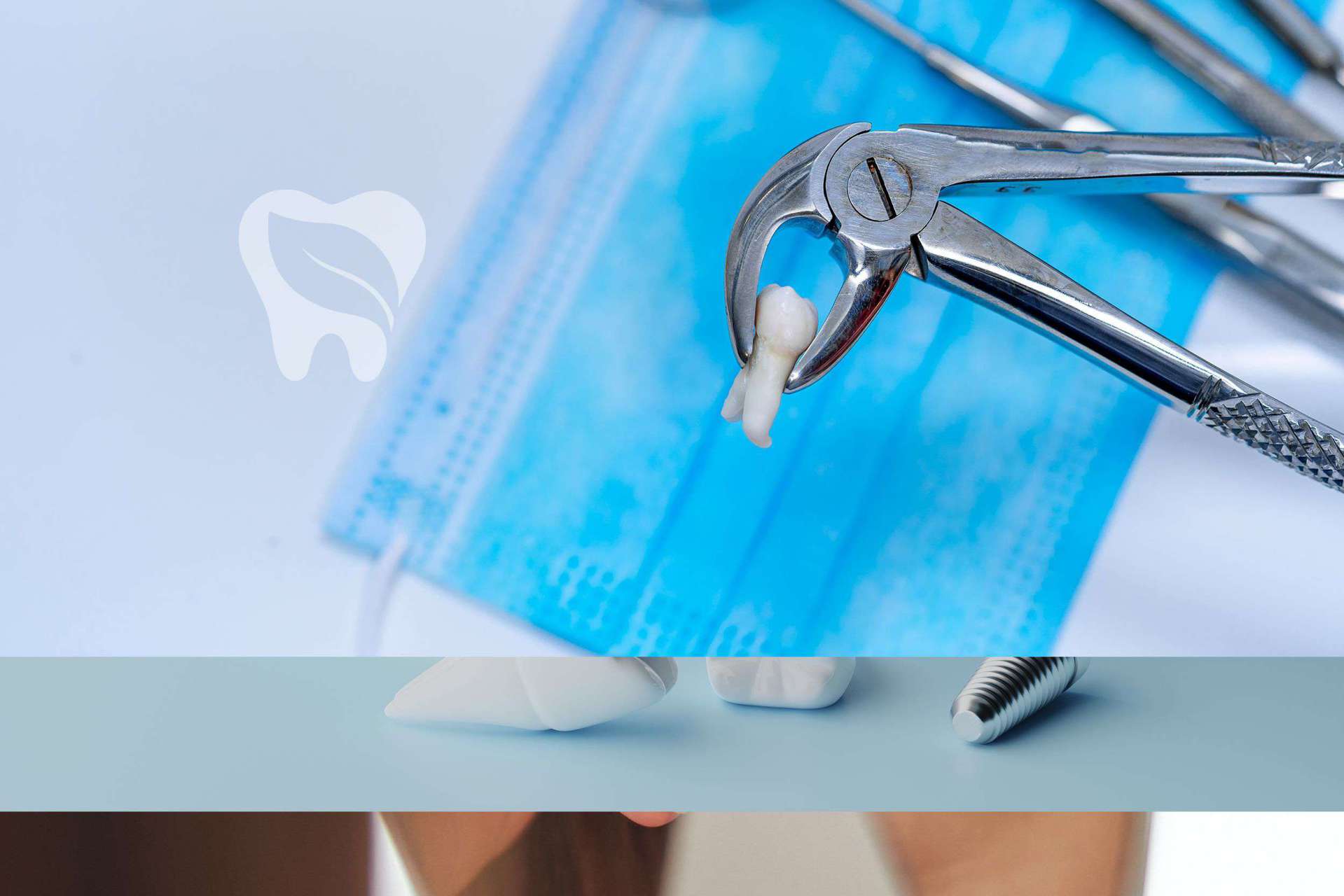
Impacted Tooth Surgery
Impacted or partially erupted wisdom teeth, canines, and other retained teeth may lead to cavities in neighboring teeth, periodontal infections, jaw pain, and orthodontic crowding. Before extraction we evaluate root anatomy and nerve-vessel proximity with panoramic radiographs and, when necessary, cone-beam CT. Minimally traumatic surgical techniques shorten recovery times and reduce complications.
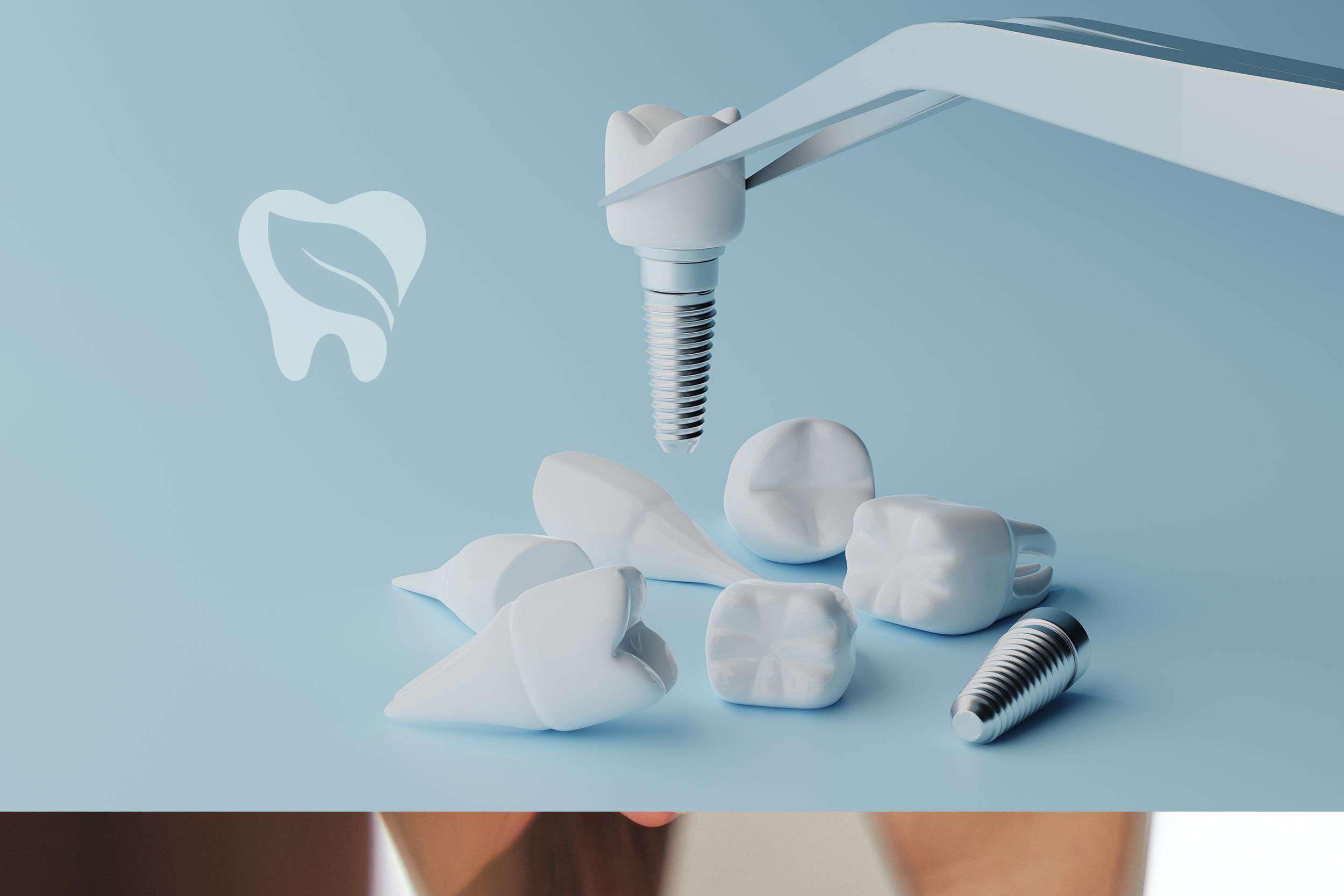
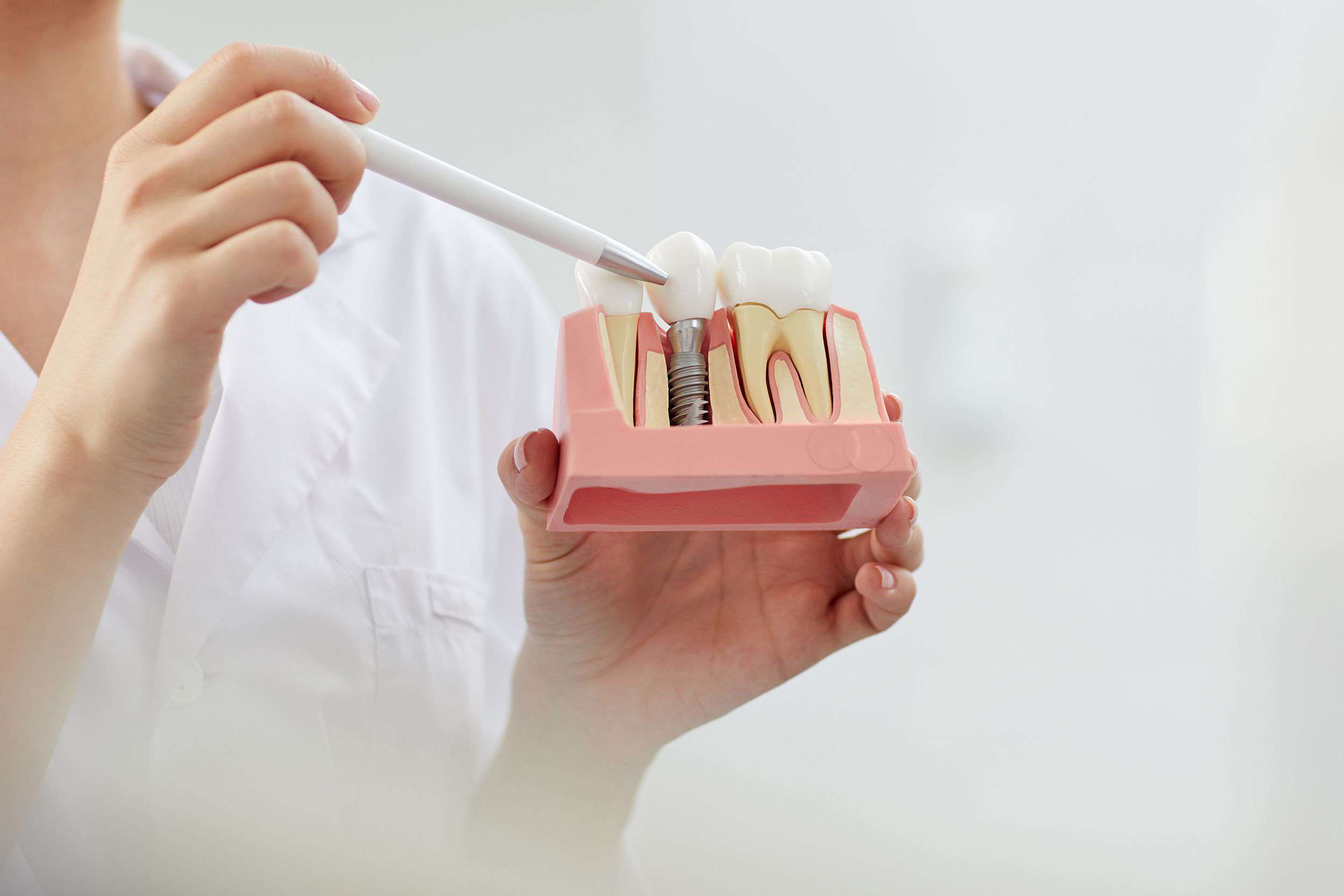
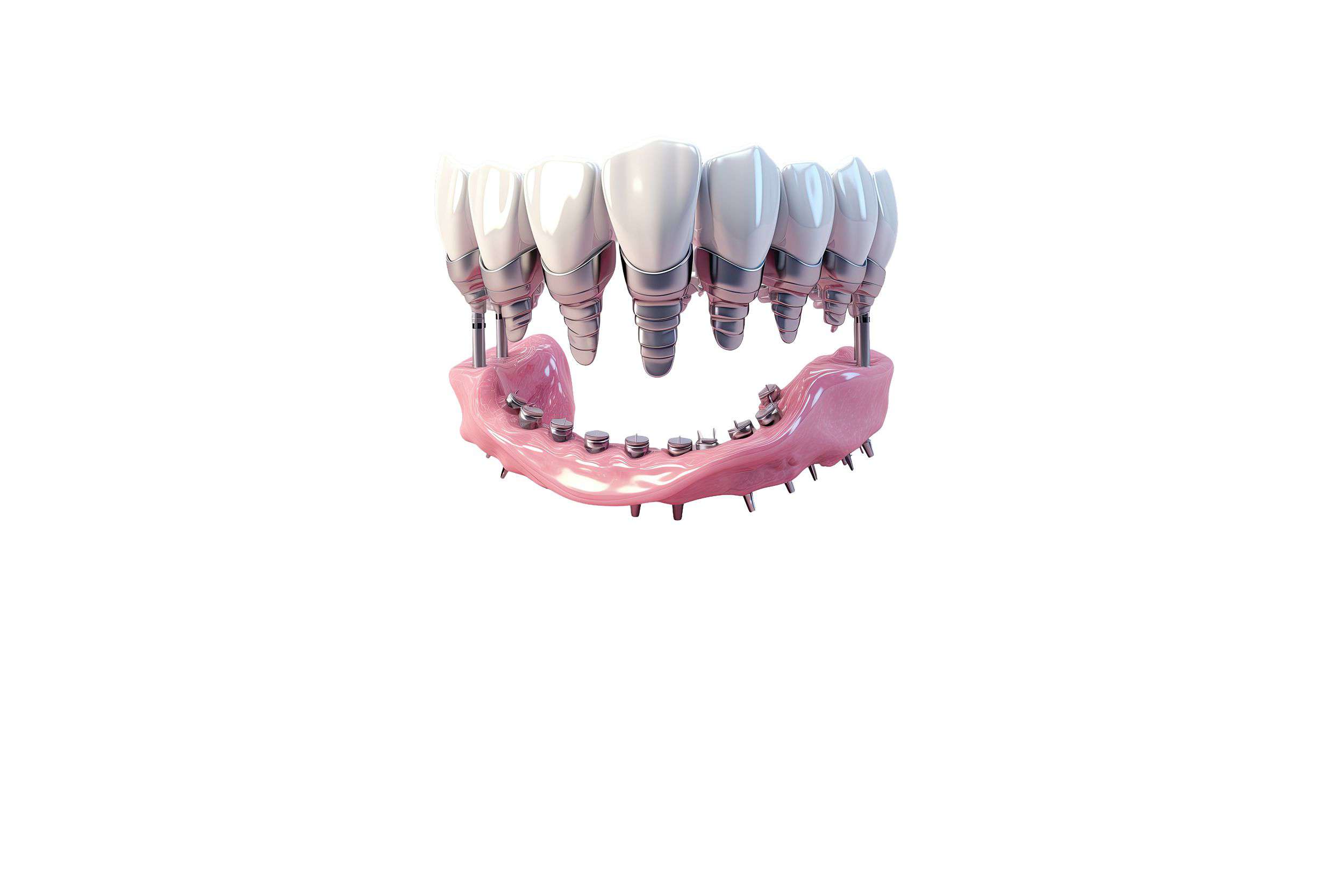
Implant Surgery
Dental implants provide long-lasting functional and esthetic replacements for missing teeth. When bone volume is inadequate we perform supportive procedures such as sinus lifts, block bone grafts, particulate grafting, membrane placement, and guided tissue regeneration. The surgical phase is enhanced with digital planning, 3D-printed surgical guides, and computer-aided smile design.
Jaw Cysts and Tumors
Odontogenic cysts, soft-tissue tumors, or bony lesions in the jaws can remain asymptomatic for long periods. Routine check-ups and radiological screenings enable early detection. Depending on the lesion type we may opt for enucleation, marsupialization, or resection, with specimens sent for histopathology. Bone regeneration and soft-tissue reconstruction follow surgery to restore the area.
Trauma Surgery
Our trauma unit treats dental and jaw fractures, soft-tissue lacerations, and temporomandibular joint dislocations. Emergency management involves stabilizing bone segments, replanting avulsed teeth, and performing primary soft-tissue repair. When indicated we use titanium plate-and-screw systems or resorbable materials for osteosynthesis.
Temporomandibular Joint Disorders
For patients experiencing joint pain, noises, limited opening, or locking we provide a broad spectrum of care ranging from conservative to surgical options. Therapies include splints, physiotherapy, botulinum toxin injections, intra-articular injections, arthrocentesis, and in advanced cases arthroscopic or open surgery.
Salivary Gland Surgery
Stones (sialolithiasis), chronic inflammations, and masses in the major and minor salivary glands are evaluated with ultrasonography and MR sialography. We plan endoscopic sialolithotomy, conservative management, or partial/total gland excision when needed, prioritizing preservation of the facial nerve during surgery.
Our Treatment Workflow
- Detailed examination and diagnosis: The first visit includes a clinical exam, thorough medical history, and digital imaging (panoramic radiograph, CBCT, intraoral scanner). Laboratory tests are ordered when indicated.
- Personalized planning: We explain each surgical step, anesthesia options, timeline, and healing expectations. Risks, alternatives, and possible complications are communicated transparently.
- Surgical execution: Procedures are carried out in sterile conditions under local anesthesia, sedation, or general anesthesia depending on the case. Tissue preservation and the use of biocompatible materials are core principles.
- Postoperative follow-up: Patients receive tailored aftercare protocols covering prescriptions, oral-hygiene instructions, and nutrition guidelines. Follow-up visits are scheduled more frequently when needed.
- Rehabilitation and support: When implants or prosthetic plans are involved, we coordinate with the prosthodontic phase. Referrals for physiotherapy or speech therapy are arranged if supportive care is required.
Benefits of Oral and Maxillofacial Surgery
- Restoring function: Chewing, speech, and facial expression are rebalanced during recovery.
- Esthetic improvement: Surgical correction of tooth and bone loss helps regain a natural smile.
- Pain and infection control: Chronic pain, infection sources, and inflammatory foci are eliminated, reducing systemic impact.
- Long-term stability: Evidence-based protocols and advanced techniques deliver durable results.
- Multidisciplinary care: Coordination with orthodontics, periodontics, prosthodontics, and radiology ensures holistic treatment.
Who Is Eligible?
We plan surgery based on systemic health, age, bone quality, and expectations. Patients with diabetes, hypertension, cardiovascular disease, or bleeding disorders are assessed in collaboration with their physicians. Elective surgery is generally postponed during pregnancy unless urgent. Cutting down on smoking improves healing. ASA classification, laboratory values, and medical consultations help determine suitability.
Sedation and Pain Management
Patient comfort is one of our top priorities. We offer:
- Local anesthesia: Effective regional anesthesia for most minor procedures.
- Conscious sedation: Intravenous or inhalation sedation administered by an anesthesiologist to help patients relax and remember little of the operation.
- General anesthesia: Selected for extensive surgeries or medical indications, performed safely with an anesthesiologist in the operating room.
- Postoperative analgesia: Prescribed analgesics, anti-inflammatory medications, and antibiotics (when needed) must be taken as directed to control discomfort.
Tips for Faster Recovery
- Apply cold compresses during the first 24 hours and avoid hot foods.
- Follow the hygiene protocol recommended by your dentist with antiseptic rinses, implant floss, and soft-bristled brushes.
- Avoid aspirin-like medications that increase bleeding risk; consult your dentist before taking any over-the-counter drugs.
- Limit smoking and alcohol, as they negatively affect bone and soft-tissue healing.
- Stay hydrated and follow a diet rich in protein and vitamins.
Frequently Asked Questions
Is swelling and pain normal after surgery?
Mild swelling and sensitivity are expected during the first few days. Cold compresses, prescribed medication, and rest help reduce symptoms quickly.
When can I return to work?
It depends on the procedure. Simple extractions may allow same-day return, while implant placement or cyst removal might require a few days of rest.
Can a prosthesis be placed immediately after implant surgery?
Immediate loading is possible when bone density, primary stability, and occlusion are favorable. Otherwise a 2–4 month osseointegration period is recommended.
Do joint noises always require surgery?
No. Conservative therapies are attempted first; surgical options are considered only for persistent cases.
When are sutures removed?
In most cases sutures are taken out during a follow-up visit 7–10 days later. Resorbable sutures may not require removal.
A Safe Surgical Experience at Yaprak Dent
Our clinics comply with international sterilization standards. Digital radiography delivers clear images with lower radiation doses, and we incorporate piezosurgery, laser applications, and advanced biomaterials during procedures. To maximize comfort we provide 24/7 communication, nutritional guidance, and medication follow-up before and after surgery. Your treatment plan is coordinated with our prosthodontic, orthodontic, and periodontal departments to achieve both esthetic and functional goals.
Book an Appointment
Contact Yaprak Dent for expert consultation, second opinions, or detailed information about planned surgical procedures. Complete the online appointment form or call our hotline to secure a same-day visit. We will guide you through individualized treatment options and payment plans—partnering with you on the path to a healthy, functional, and esthetic smile.